By Christopher J. Rutty, Ph.D.
Professional Medical/Public Health Historian
Adjunct Professor, Dalla Lana School of Public Health, University of Toronto
Confluence: November 8, 1920
The start of Santa Barbara’s “Insulin Era” depended upon the coincidence of three events occurring on November 8, 1920; two in Santa Barbara, and a third, some 2,600 miles to the northeast, in Toronto, Ontario, Canada.

Also, on November 8, 1920, another person suffering from advanced diabetes, Charles Cowan, a 51-year-old man from Anaheim, California, was admitted to the Potter Metabolic Clinic, which had become part of the Santa Barbara Cottage Hospital a year earlier. This clinic was originally established by Dr. Nathan B. Potter in 1916-17 in New York City as the “Memorial Laboratory and Clinic for the Study and Treatment of Nephritis, Gout and Diabetes.” A specialist in metabolic diseases, Dr. Potter was stricken with diabetes himself in 1911, and in 1916, his daughter, Mary, died of a rare form of leukemia following an intensive effort to save her. As a memorial to his daughter, Dr. Potter gathered financial support from the Carnegie Corporation, along with other subscribers, to establish the Memorial Lab and Clinic at New York City Hospital.

On November 8, 1920, Dr. Frederick G. Banting first met Professor J.J.R. Macleod in the University of Toronto Physiology Department. Banting was eager to pursue a compelling idea he had about an experimental method to isolate the elusive internal secretion of the pancreas, the use of which might provide some relief against diabetes. Macleod was skeptical about the idea and about Banting’s qualifications for understanding diabetes and for exploring the idea in a research laboratory. However, based on Banting’s medical training at the University of Toronto, his clear skills as a surgeon, demonstrated most notably during his war service, as well as his bold perseverance, Macleod decided to give Banting a chance, not so much because of the potential of the idea, but because negative results would also prove illuminating. From this November 8, 1920, meeting a series of events were set in motion that would lead to the discovery of insulin, reaching a climax with its first successful human use on a severe diabetic patient, 13-year-old Leonard Thompson in January 1922.[1]

However, before the clinic was completed, and to better support Dr. Potter’s declining health, it was suggested a superior location for the clinic would be in the warmer climate of southern California, and specifically Santa Barbara, which had developed a reputation as a health center. The Santa Barbara Cottage Hospital, which opened in 1891, was supportive of accommodating what would be called the “Potter Metabolic Clinic.”

In the fall of 1917, Dr. Potter was a dying man when he arrived in Santa Barbara to begin building the clinic. His resilience impressed wealthier members of the Santa Barbara community, prompting funds to support the construction of the Potter Metabolic Wing. However, by the summer of 1919, with the new wing half built, Potter’s health rapidly declined, and he died on July 5, 1919. The Potter Metabolic Wing officially opened on October 25, 1919, and by September 1920, it was clear a prominent diabetes specialist was needed to lead the clinic. The perfect candidate seemed to be Dr. William David Sansum (1880-1948), who had been a research scientist at Presbyterian Hospital in Chicago. It did not take long for Dr. Sansum to accept the offer and on November 8, 1920, his train from Chicago pulled into the Santa Barbara station.[2]


[2] Walker A. Tompkins, Continuing Quest: Dr. William David Sansum’s Crusade Against Diabetes (Santa Barbara: Sansum Medical Research Foundation, 1977). See also: Erin T. Graffy and Erno S. Daniel, “Sansum Clinic: A Legacy of Medical Innovation,” Noticias: Journal of the Santa Barbara Historical Museum 54 (2) (2014): 61-113, https://issuu.com/santabarbaramuseum/docs/sansumnoticiasfinal/25
On May 17, 1921, in a small lab in the Medical Building at the University of Toronto, Frederick Banting began the pancreatic extract research work with the assistance of Charles H. Best, who had just completed the Physiology and Biochemistry undergraduate program taught by Macleod. Despite the summer heat and a variety of challenges, by early August, Banting and Best were able to prepare an extract from the pancreas of a healthy dog that reliably reduced the sugar levels in the blood and urine of another dog made diabetic after the removal of its pancreas. On November 14, 1921, Banting and Best gave their first presentation about their work to the Physiology Department’s Journal Club, this paper forming the basis of their first publication, “The Internal Secretion of the Pancreas,” which appeared in the February 1922 issue of The Journal of Laboratory and Clinical Medicine.[3] Between the Journal Club presentation and the appearance of the first publication, word began to spread among diabetes specialists about the Toronto pancreatic extract research, soon reaching Dr. Sansum in Santa Barbara.



[4] Tompkins, p. 29.
Dr. William D. Sansum and Diabetes
William Sansum had wanted to be a doctor from an early age. He would ultimately find his niche in medical research and become one of the most respected medical research scientists in the United States in the field of metabolic diseases. His special interest in diabetes solidified during his Ph.D. studies, his dissertation titled, “Studies on the Theory of Diabetes Mellitus.” During his first year in Santa Barbara, Dr. Sansum continued the diabetes research he had pursued in Chicago, focused on developing a chemical compound that might duplicate in the lab the pancreatic secretions otherwise missing or deficient in the metabolism of the diabetic patient. Sansum published five papers during his first year at the Potter Clinic on various aspects of diabetes, while also overseeing the care of some 175 patients in the clinic, 58 of whom were diabetic; they came from across the U.S. and some from Canada. Dr. Sansum was well-liked by his patients and in the community. He became known as “Father Sansum” after taking a group of diabetic children to a downtown theater for a Saturday matinee. When he approached the box-office with his “family”, the cashier would say to the doorman, “Here comes Father Sansum,” and the name stuck.[4]
Making Insulin in Santa Barbara, Phase 1: February – May 1922
When Sansum read Banting and Best’s first publication in late January/early February 1922, he was likely not yet aware that the first successful human test of the pancreatic extract had just taken place in Toronto. There had also been several important developments with the extract since their paper was accepted for publication, most notably the discovery that the extract could be prepared from adult beef pancreas rather than relying on canine pancreas tissue as was described in the first paper.[5]
However, based on a close reading of that first paper, coupled with his own diabetes research experience, the lab facilities and support available at the Potter Clinic, and the urgency of many severe diabetic cases under his care, Sansum made a bold proposal to his colleagues, Dr. Norman Blatherwick (chief chemist) and Dr. Marion Bell (lab chemist). “In my judgement, the Canadian reports offer a greater promise of success that our attempts [to compound a biochemical substitute for insulin]. Our clinic is admirably equipped to attack out problem from Banting’s angle, don’t you think!” Blatherwick agreed. “What they can do in Canada, we should be able to duplicate in Santa Barbara. And improve on.” Sansum was pleased with the support. “I feel justified in ordering an entirely new line of work here. Using Banting and Best’s techniques, we will attempt to manufacture our own insulin from animal glands.”[6] Sansum’s first challenge was finding a dependable supply of fresh canine pancreas glands, although the local dog pound would not be the answer, especially amid vocal anti-vivisection sentiments in the community.

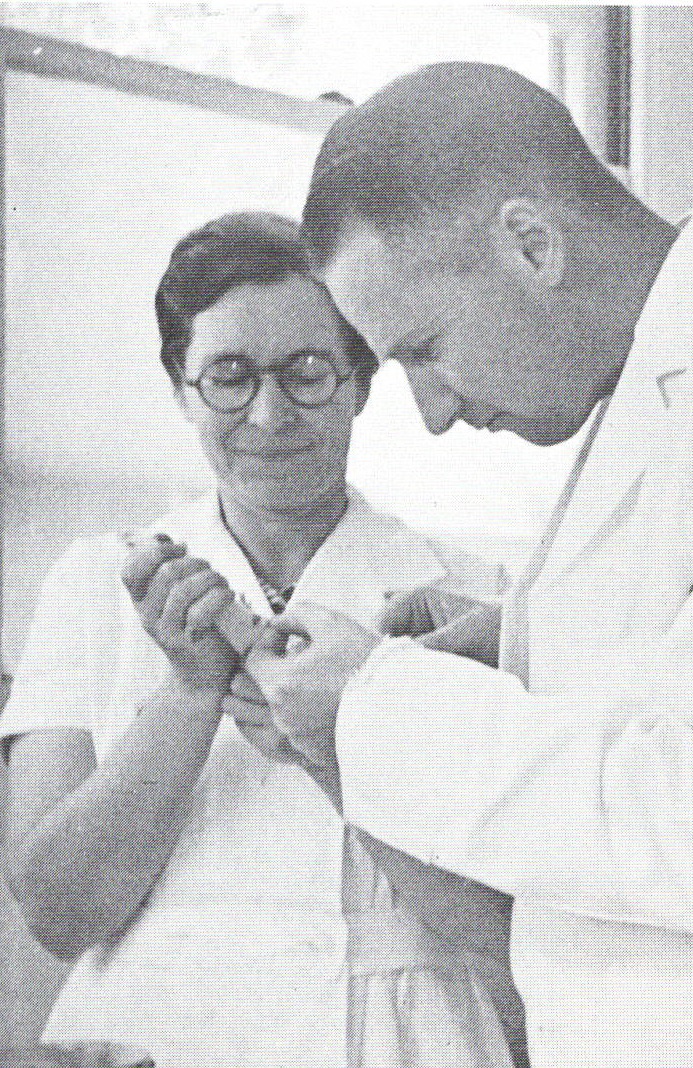
Fortunately, by early March, news arrived from Toronto of the recent developments with bovine pancreas as a source of extract. Such tissues were plentiful and otherwise discarded in the meatpacking industry. As work in Santa Barbara began, Sansum corresponded with Banting, although at the time, production of the extract in Toronto at the university’s Connaught Antitoxin Laboratories had slowed to a trickle just as the Toronto group’s publication on the first clinical tests of the extract appeared in the March 1922 issue of the Canadian Medical Association Journal. At the same time, the front-page headline of the Toronto Star of March 22nd announced, “Toronto Doctors on Track of Diabetes Cure.” The juxtaposition in Toronto between the positive news, and the practical challenges involved with moving from small to larger scale production of the extract, was especially difficult for Banting. However, by late April, after an intensive effort by the full Toronto team, the extract production challenges were largely resolved.[7] As Banting told Sansum in an April 25th letter, “I may say that had it not been for an unforeseen hold-up in which we lost the method entirely and had to commence all over, it would have been in print before now.”[8] Banting was referring to a second publication he prepared with Best, “Pancreatic Extracts,” published in the May 1922 issue of The Journal of Laboratory and Clinical Medicine.[9]
The appearance of this article coincided with a seminal presentation given by Macleod at a major conference in Washington, D.C. on May 3rd which detailed the latest clinical experience in Toronto with what was now officially called “insulin.” The conference was attended by leading diabetes specialists in North America and sparked an intensifying interest in insulin and in demand for it. However, it was clear that the insulin supply from Toronto would remain very limited for some time. In June, to expedite the development of larger scale production methods, the Toronto group began a one-year research and development partnership with Eli Lilly & Co. of Indianapolis. At the same time, the Toronto group, led my Macleod, encouraged localized efforts to prepare insulin on an experimental scale in support of a careful program of development and clinical evaluation.[10] The work led by Dr. Sansum in Santa Barbara was the first, most ambitious, and the most successful of such localized efforts in North America.

The initial challenge Sansum faced was securing a supply of beef pancreas. He first approached Santa Barbara’s leading meat wholesaler/retailer, R.N. Gehl, which operated a slaughterhouse on the west side of town. However, just as Sansum approached the firm, local community pressure over the malodorous conditions near the slaughterhouse forced its relocation seven miles further west. Nevertheless, the owner of the firm was happy to supply pancreas tissue at no charge in support of diabetes research. The fresh pancreas tissues would have to be carefully collected. Thus, during most of April, Sansum got up at 3:00 a.m. each morning to be at the slaughterhouse, ice chest in hand, ready to collect pancreas tissue. Sansum also had to drive to Los Angeles once-a-week to secure hog, sheep, and steer pancreas while Gehl’s slaughterhouse relocated. Excited to a level he had not experienced since his first dissections as a medical student, Sansum passed the first batch of beef pancreases to Dr. Blatherwick and his lead lab assistant, Loyal C. Maxwell, in the Potter Metabolic Wing. Lab technician, Melville Sahyun performed the assay to measure potency of the extract, testing it against a master sample sent from Toronto. The first potency test was surprisingly good, but not the second, prompting extensive lab experimentation to isolate the problem.
By the end of May, Sansum’s insulin seemed ready to test on a human diabetic. Several diabetic patients in Toronto had been successfully treated with insulin prepared by the University of Toronto’s Connaught Laboratories. In addition, Jim Havens, a 22-year-old man from Rochester, NY, on May 21, became the first in the U.S. to receive insulin. Havens was treated with insulin sent from Toronto, including some personally delivered by Banting.[11]
On May 31, 1922, Charles Cowan was very close to death. His condition had declined since his admission to the Potter Metabolic Clinic on November 8, 1920. To Sansum, the time seemed right to test his insulin on a diabetic patient and Cowan would not otherwise live much longer. On May 31st Cowan was given an insulin injection of 3 c.c., but his initial urine tests on June 1st showed that sugar was still present, as was also the case on June 2nd. However, by the third day after his initial insulin injection, Cowan had much better tests and was on the road to recovery. The other diabetic patients in the clinic shrieked with joy as it looked like their death sentences had been lifted. However, to ensure death sentences were not reimposed, the challenge for Sansum’s team was to ensure the insulin supply continued.

[5] C.J. Rutty, “It works! Now what?” https://definingmomentscanada.ca/insulin100/history/it-works-now-what/
[6] Tompkins, p. 35.
[7] See C.J. Rutty’s articles for Defining Moments Canada Insulin 100, “History of Connaught,” https://definingmomentscanada.ca/insulin100/history/connaught/; “Making Insulin,” https://definingmomentscanada.ca/insulin100/history/making-insulin/; “The Discovery Goes Public,” https://definingmomentscanada.ca/insulin100/history/the-discovery-goes-public/
[8] Tompkins, p. 43.
[9] The article is available at: https://insulin.library.utoronto.ca/islandora/object/insulin%3AT10003
[10] See C.J. Rutty’s articles for Defining Moments Canada Insulin 100, “Patent Protection,” https://definingmomentscanada.ca/insulin100/history/patent-protection/; “Eli Lilly,” https://definingmomentscanada.ca/insulin100/history/eli-lilly/
[11] See C.J. Rutty’s Defining Moments Canada Insulin 100 article, “Diabetic Resurrections,” https://definingmomentscanada.ca/insulin100/history/diabetic-resurrections/
Making Insulin in Santa Barbara, Phase 2: June – September 1922
Sansum wrote a detailed letter to Macleod on June 15, highlighting the progress being made in Santa Barbara, based on the recent work in Toronto, and the very optimistic reaction among prominent diabetes specialists to Macleod’s presentation in Washington. Sansum noted that his team had been able to make potent extracts from beef, calf, and sheep pancreas, but not from hogs, and had tested them on Cowan, who was “a thoroughly reliable and trustworthy man.” Based on the initial small-scale success and the need to prepare larger amounts of insulin, an arrangement was made with the Hauser Packing Company of Los Angles to secure fresh pancreas tissue, although for some reason, they were not yielding potent extract.[12] As soon became clear, insulin potency related to the time between when the animal was fed and when slaughtered and the pancreas collected; the more recently they were fed the better.


In his June 21st reply, Macleod was clearly impressed with the progress being made in Santa Barbara. Macleod sent Sansum a copy of Connaught Labs’ latest directions for insulin production, and he noted that the Toronto group had established a partnership with Eli Lilly & Co. of Indianapolis, to work on quantity production. While Macleod was “delighted to have you do what you can to prepare extract,” he emphasized to Sansum, “The only thing in connection with the preparation that in justice to Eli Lilly Co., we must safe-guard is that no other commercial firm should, at present, obtain knowledge of the method we are using. You will therefore, for the present at least, keep the information I have given you for private use entirely.”[13]
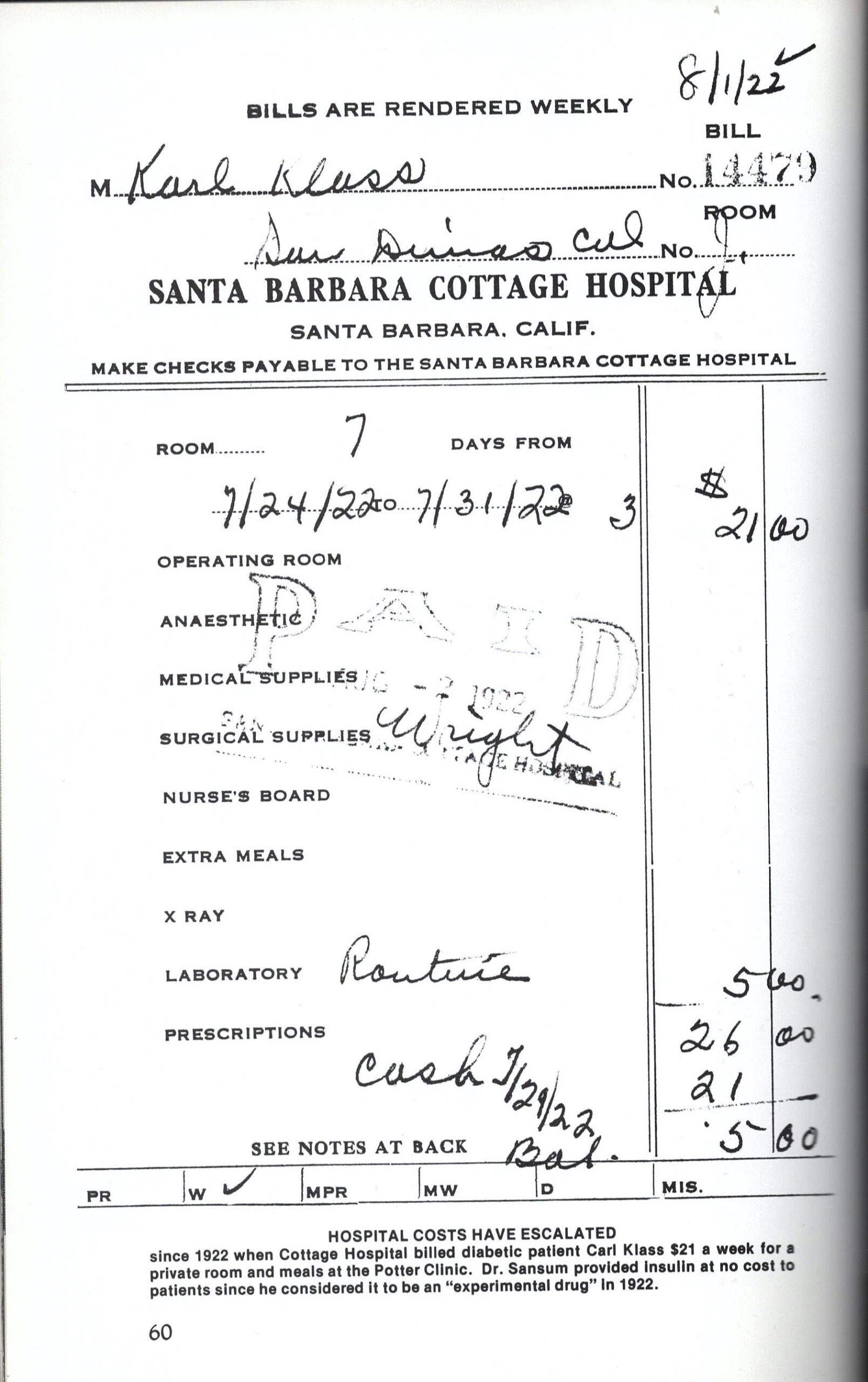
A month later, Sansum was pleased to report to Macleod that, “We have had no difficulty in the production of Insulin by your method.” The extracts had been very potent and enabled “three very convincing, human experiments.” In addition to Cowan, insulin treatments had been given to a Mrs. D., age 53, who was a more severe case than Cowan, as well as to the “emergency case” of a 12-year-old boy, Carl Klass, “sent to us by a good man in Los Angeles.” Sansum also experimented with the oral administration of Insulin by mixture with wine, or in a capsule form, but neither test had any measurable effect.[14] During August, however, Sansum encountered challenges with maintaining stable potency levels, particularly with insulin prepared from pancreas tissues obtained from the Los Angeles meatpacking plant. He was also concerned about the costs the clinic was incurring in producing insulin and providing it at no charge. Sansum had already paid some $1,400 out of his own pocket to provide free insulin to his patients.
Sansum was also anxious to publish about the clinical results of insulin treatment so far, but Macleod asked him not to. As explained in an August 27th letter, Macleod asked Sansum “to withhold publication of your most interesting clinical results until Dr. Banting
and the others associated with him in Toronto have had a reasonable time to complete their work in the clinic.” Furthermore, “It would involve me in serious misunderstandings with my associates if you were to publish ahead of them, especially since you and Woodyat were the only persons to whom I sent manuscript copy of the paper on methods of preparation of Insulin.”[15] Macleod also suggested Sansum visit Toronto to further discuss the Santa Barbara work at a meeting of the University of Toronto’s Insulin Committee. Sansum had planned to take some time off to go fishing, but, after hearing from Macleod, decided to board a train for Toronto. After fruitful meetings with Macleod and Banting, as well as a visit to Connaught’s insulin production facility, Sansum was back in Santa Barbara by September 17. By this time, Sansum had arranged a program of regular testing of insulin prepared by Eli Lilly (which it called “Iletin”). There would be enough Iletin (100 units/week) sent from Eli Lilly for clinical tests involving “one of our carefully measured cases.”[16] Such tests were important in revealing inconsistencies in potency of Lilly’s Iletin compared to insulin produced in Santa Barbara.
[12] W.D. Sansum to J.J.R. Macleod, June 15, 1922, https://insulin.library.utoronto.ca/islandora/object/insulin%3AL10248
[13] W.D. Sansum to J.J.R. Macleod, July 21, 1922, https://insulin.library.utoronto.ca/islandora/object/insulin%3AL10250
[14] J.J.R. Macleod to W.D. Sansum, June 21, 1922, https://insulin.library.utoronto.ca/islandora/object/insulin%3AL10249
[15] J.J.R. Macleod to W.D. Sansum, Aug. 27, 1922, University of Toronto Archives (UTA), A1982-0001, Box 13, file 13.
[16] Meetings, University of Toronto Insulin Committee, Sept. 1 and Sept. 22, 1922, https://insulin.library.utoronto.ca/islandora/object/insulin%3AW10028; W.D. Sansum to J.J.R. Macleod, Sept. 26, 1922, UTA, A1982-0001, Box 13, file 13.
Soon after returning from Toronto, Sansum met with Henry F. Pritchett of the Carnegie Corporation to discuss financial support for the Potter Metabolic Clinic’s experimental insulin production and clinical work that could add to the initial support Carnegie provided to the clinic. Impressed with the insulin work in Santa Barbara, Pritchett immediately pledged a grant of $15,000. On October 8, a prominent New York Times article about the Carnegie grant appeared, which included details about the insulin work going on in Santa Barbara, prompting a flood of letters from desperate diabetics hoping to receive insulin. In response, on October 16, Sansum issued a general statement summarizing the effectiveness of insulin with the limited number of severe diabetic patients at the Potter Clinic, but that there was a very limited supply. Insulin was not for sale in Santa Barbara and the ongoing experimental work was being financially supported by generous contributions. Only the severest cases could be accepted for insulin treatment, but it was expected there would be an ample commercial supply of insulin available within the next six months to a year.[17] At the time, Sansum’s team was making enough insulin to enable regular treatment of 14 patients.
[17] W.D. Sansum, “General Statement,” Oct. 16, 1922, UTA, A1982-0001, Box 13, file 13.


Making Insulin in Santa Barbara Phase 3: October – December 1922
Increased public attention to the experimental insulin work in Santa Barbara put further pressure on Sansum and the Potter Clinic’s limited facilities to increase production, which included frequent trips to the meatpacking plant in Los Angeles. Sansum often drove the 200-mile round trips personally to retrieve pancreas tissues, the proper transport of which required they be kept in large amounts of grain alcohol. However, the early 1920s was a time of prohibition in the United States on the manufacture, sale, and transport of intoxicating liquors. Prohibition had come into effect in January 1920 with the implementation of the 18th Amendment to the U.S. Constitution and would continue until 1933.
One day in November 1922, while making the return trip from Los Angeles carrying pancreases immersed in alcohol, Sansum was pulled over by the police and given a ticket for transporting alcohol, thus violating prohibition laws. The cargo of pancreases in alcohol was impounded, threatening the further production of insulin. Frustrated at the arbitrary application of the law, Sansum was unsure what to do. An opportunity emerged in early December when he read about Elizabeth Hughes, daughter of the U.S. Secretary of State, Charles Evans Hughes, returning home to Washington, D.C. after being successfully treated with insulin in Toronto.[18] Sansum immediately wrote a long letter to Secretary of State Hughes, appealing for help to resolve the impounded pancreases and alcohol situation. Immediately after reading the letter, Hughes phoned the Secretary of the Treasury, whose department was responsible for the Prohibition Laws. Very shortly thereafter, Sansum received a telegram signed by Hughes. The telegram affirmed that the Treasury Department had granted permission for Sansum to purchase and transport as much alcohol as he might require for the insulin work and all charges were dropped.
[18] See C.J. Rutty’s Defining Moments Canada Insulin 100 article, “Elizabeth Hughes: Letters From Toronto,” https://definingmomentscanada.ca/insulin100/history/elizabeth-hughes-letters-from-toronto/
When Sansum wrote to Macleod on January 13, 1923, he “had very little to report to you along the line of advancement in our experimental manufacture of Insulin, in fact the harder we seem to work, the more money we spend and the more glandular material we use, the smaller becomes our proportional yield. We are, of course, manufacturing more Insulin than ever before but the yield in proportion to our efforts is certainly very discouraging.” And while there had been progress with the treatment of clinic cases with insulin, especially near-fatal cases, Sansum told Macleod, “Many patients no longer write in ahead for accommodations but present themselves in the last stages of the disease and we are forced to admit them often time putting two patients in a private room.”[19] Medical and public attention to Sansum’s insulin work led to several invitations for him to speak at medical meetings, but he was careful to get Macleod’s approval. For example, after Sansum told Macleod of an invitation to speak at the annual meeting of the Southern California Medical Society in early April, Macleod approved, noting “The papers from the clinics here will have been published by that date so there is no reason why you should not present the subject in your community.”[20] More generally, there was an urgent need to educate physicians across the country about the use of insulin. As Sansum stressed in a letter to Macleod in mid-February, “We are constantly afraid that by over-dosing some patient, a needless death may occur which would seriously injure this great discovery.”[21]
By this time, 70 cases of diabetes had been treated with insulin produced in Santa Barbara, supplemented with some Lilly Iletin for experimental tests. Ten patients had returned home, either able to manage their diabetes through diet alone, or were unable to afford to buy Iletin. Another 10 were home and supplied with Iletin, while another 10 were receiving Iletin paid for my Sansum. There had been 5 cases of diabetic coma, two of which had been revived with insulin and were doing well, while three died.
As Sansum emphasized to Macleod, costs were mounting rapidly. The first cases were treated at a cost of about $100 per patient day; by August-September, the cost was down to $10 per patient day and by February 1923, was close to $3.00 per patient day.

However, “With every increasing number of severe cases reaching a stage where we must make some charge to patients to cover at least part of the experimental cost or go into bankruptcy.” It had never been Sansum’s intention “to let any patient go without insulin because he has no money.” Some funds had recently been donated to help with some of the needy patients. Sansum planned to continue with experimental manufacture of insulin, but “only until such time when an ample commercial supply is available at a fairly reasonable rate.”[22]
Sansum knew insulin was a patented process and that it was being prepared in Santa Barbara without a license, but with the University of Toronto’s full knowledge and consent. However, he had to ask Macleod if some charge could be requested “for our product in proportion as patients can afford to pay for it.” Would it also “be permissible to secure a fund, as I believe I can, to assist the worthy, needly patients who cannot afford to pay a minimum cost price?”[23] After consulting with the Insulin Committee, Macleod quickly replied with answers of yes to both of Sansum’s questions. As he explained, “At present it is quite unnecessary for us formally to issue you a license under the patents to carry on this work, the only understanding being that none of the Insulin manufactured by you is sold in the open market.” Furthermore, “The University also heartily approves of any scheme you may devise for supplying insulin to worthy needy patients who cannot afford to pay for it.”[24] By the end of February, Sansum was happy to tell Macleod that a fund of $10,000 had been raised for use as “as a sort of subsidy to patients who cannot afford to pay the market price for Iletin. They will be permitted to pay what they can. The difference will be charged to this fund.”[25]
By mid-April 1923, Sansum was pleased to report to Macleod that the clinic was purchasing an increasing amount of Iletin, while “using more of our product for experimental study.” This amounted to some 10,000 units/week for clinic patients, and considerably more supplied by Lilly for patients that had been sent home. “Our clinical results continue to be wonderful as you would suppose and we now have 100 cases.” However, so far, “all our efforts at mouth medication have been frank failures even when we have given by mouth as high as 25 times the hypodermic dose.”[26]
[19] W.D. Sansum to J.J.R. Macleod, Jan. 13, 1923, UTA, A1982-0001, Box 13, file 13.
[20] J.J.R. Macleod to W.D. Sansum, Feb. 5, 1923, UTA, 1982-0001, Box 13, file 13.
[21] W.D. Sansum to J.J.R. Macleod, Feb. 15, 1923, UTA, 1982-0001, Box 13, file 13.
[22] W.D. Sansum to J.J.R Macleod, Feb. 16, 1923, UTA, 1982-0001, Box 13, file 13.
[23] Ibid.
[24] J.J.R. Macleod to W.D. Sansum, Feb. 22, 1923, UTA, A1982-0001, Box 13, file 13.
[25] W.D. Sansum to J.J.R. Macleod, Feb. 28, 1923, UTA, 1982-0001, Box 13, file 13.
[26] W.D. Sansum to J.J.R. Macleod, Apr. 13, 1923, UTA, 1982-0001, Box 13, file 13.


The end of the “Insulin Era” in Santa Barbara happened in two stages, the first caused by a major epidemic of hoof-and-mouth-disease during the spring of 1924 that infected cloven-hoofed animals, including herds of cattle, sheep, and hogs. It was highly contagious and required a strict quarantine and mass cremations of diseased animals and forced the closure of slaughterhouses. The situation was catastrophic and led to the curtailment of all insulin work in Santa Barbara. The crisis soon passed, and insulin work resumed in Santa Barbara with an increasing focus on a variety of research projects, especially related to diet management and to further studies on oral administration of insulin, accommodated in additional lab space created under the former maternity wing of the hospital.[27] During 1924 there had been a doubling of patient volume to just under 500 patients in the clinic, with 151 diabetics, but the broader commercial availability of insulin (mostly from Eli Lilly, but with several other U.S. firms starting production) relieving insulin production pressures in Santa Barbara. During this period, Sansum’s persistence in searching for a way to administer insulin orally would be his greatest frustration, while his research on diet management of diabetes his greatest success.
The second and ultimately fatal blow to Santa Barbara’s “Insulin Era” came on June 29, 1925, when a major 6.3 earthquake shook the Santa Barbara area.[28] The quake resulted in 13 deaths and major damage to the city’s downtown core, but it caused only minimal damage to the hospital and Potter Wing. Santa Barbara’s other two hospitals suffered heavy damage, forcing the transfer of many patients to the Cottage Hospital, where most were cared for in tents until the building’s safety was checked. Amidst the post-earthquake turmoil and aftershocks, producing insulin would become an especially onerous chore. Fortunately, by 1925, Eli Lilly, along with several other U.S. firms, were able to supply enough standardized, high-potency insulin to enable Sansum to finally halt the Potter Clinic’s insulin manufacturing program permanently. A Sansum’s biographer concluded, “After five years of predawn visits to slaughterhouses, gruelling round trips to Los Angeles, and tedious extraction and assay work in the laboratory, Dr. Sansum was only too glad to announce the passing of Santa Barbara’s historic ‘insulin era.’”[29]



[28] https://www.sbhistorical.org/quake-the-1925-earthquake-in-santa-barbara/
[29] Tompkins, p. 103.
Photo Sources:
[31] Image 2 source: Sanofi Vaccines Canada (Connaught Campus) Archives, Toronto
[32] Image 3 source: Sanofi Vaccines Canada (Connaught Campus) Archives, Toronto
[33] Image 4 source: https://sansum.org//about-us/
[34] Image 5 source: W.A. Tompkins, Continuing Quest, p.55
[35] Image 6 source: Tompkins, p. 56
[36] Image 7 source: Tompkins, p. 57
[37] Image 8 source: https://insulin.library.utoronto.ca/islandora/object/insulin%3AP10043
[38] Image 9 source: https://insulin.library.utoronto.ca/islandora/object/insulin%3AP10090
[39] Image 10 source: Tompkins, p. 53
[40] Image 11 source: Tompkins, p. 57
[41] Image 12 source: Tompkins, p. 57
[42] Image 13 source: https://insulin.library.utoronto.ca/islandora/object/insulin%3AC10025
[43] Image 14 source: Tompkins, p. 57
[44] Image 15 source: https://insulin.library.utoronto.ca/islandora/object/insulin%3AP10031
[45] Image 16/16a source: https://insulin.library.utoronto.ca/islandora/object/insulin%3AL10248
[46] Image 17 source: https://insulin.library.utoronto.ca/islandora/object/insulin%3AL10249
[47] Image 18 source: Tompkins, p. 60
[48] Image 19 source: Author
[49] Image 20 source: Author scan (University of Toronto Archives, A1982-0001, Box 13, file 13
[50] Image 21 source: https://insulin.library.utoronto.ca/islandora/object/insulin%3AC10066
[51] Image 22 source: Author scan (University of Toronto Archives, A1982-0001, Box 13, file 13
[52] Image 23 source: Author scan (University of Toronto Archives, A1982-0001, Box 13, file 13
[53] Image 24 source: Author scan (University of Toronto Archives, A1982-0001, Box 13, file 13
[54] Image 25 source: Author
[55] Image 26 source: Tompkins, p. 63
[56] Image 27 source: Tompkins, p. 59

